Services
Comprehensive RCM Services Built for Healthcare’s Complexity
From patient access to final payment, our end-to-end revenue cycle solutions are designed to improve efficiency, ensure compliance, and maximize financial performance, so your organization can thrive in a changing healthcare landscape.
Why Providers Trust MedStat’s RCM Services
Revenue Cycle Solutions
That Adapt to You
At MedStat, we don’t believe in one-size-fits-all. Our RCM solutions are designed to integrate with your existing workflows or implement a full-service model, whichever works best for your team. Whether you’re a small practice or a large healthcare network, MedStat delivers billing and collections that are fast, flexible, and built for today’s challenges.
Offload Staffing Headaches
Let our team handle the heavy lifting so you can focus on care, not coverage.
Strengthen Coding & Compliance
Meticulously preparing and submitting claims to payers for services provided.
Minimize Denials and Errors
Listening to and addressing reasons for claim denials to secure rightful reimbursements.
Improve Patient Collections
Clear, compassionate communication helps patients understand and resolve balances, faster.
Modernize Legacy AR Systems
We help you clean up aging A/R and ensure nothing falls through the cracks when platforms change.

Our Services
MedStat Revenue Cycle Management Services
Whether we integrate with your existing system or implement one of our billing partners, you’ll get a solution that’s customized, compliant, and optimized to recover more revenue with less friction.
MedStat brings more than manpower. The 6th sense of RCM goes beyond the basics, combining smart automation, predictive analytics, and proactive problem-solving to drive measurable results. We optimize every stage of the revenue cycle, from patient access and charge capture to denial management and collections, with workflows designed to reduce errors, accelerate reimbursements, and improve financial performance. Traditional vendors react to problems; we anticipate them and resolve them before they impact your bottom line.
Billing & Coding
We manage billing and coding as a single, tightly controlled workflow to eliminate handoff errors and revenue leakage. Our certified teams apply payer-specific rules, specialty logic, and multi-level QA to ensure clean claims the first time. The result: faster reimbursement cycles, fewer audits, and consistently higher net collections without burdening your staff.
AR & Coding Backlogs
Backlogs hide real cash, and we are built to unlock it quickly. We deploy focused recovery teams supported by analytics that prioritize high-value and time-sensitive accounts first. By correcting root causes while working inventory, we don’t just clear backlogs, we prevent them from returning.
Charge Entry
Charge entry errors create downstream denials that are expensive to fix. Our process combines expert chart review, specialty-specific coding logic, and real-time validation to ensure every service is captured accurately and on time. This precision reduces rework, accelerates billing, and protects revenue from day one.
Collections
We recover patient balances early, before accounts age and relationships suffer. Our approach blends respectful, patient-friendly outreach with digital engagement and smart prioritization. You collect more, faster, while preserving patient trust and minimizing internal follow-up workload.
Pre-Authorization
Authorizations are one of the most common, and costly points of revenue failure. We manage the entire authorization process with payer-specific expertise, ensuring medical necessity, documentation, and timing requirements are met before services are rendered. This prevents avoidable denials, reduces reschedules, and protects revenue before the claim is ever created.
AR Follow-Up
AR follow-up isn’t about chasing balances, it’s about disciplined execution. We actively manage claims from submission through resolution, intervening at the optimal moment based on payer behavior and claim risk. This proactive approach shortens AR days, reduces write-offs, and stabilizes cash flow.
Denial Management
Denials are signals, not setbacks. We analyze every denial for root cause, appeal aggressively when warranted, and implement process fixes to stop repeat issues. Our denial strategy improves recovery today while structurally lowering denial rates tomorrow.
Pre-Registration
Clean revenue starts before the patient arrives. We ensure accurate demographics, real-time eligibility verification, authorization checks, and clear financial responsibility upfront. This prevents avoidable denials, accelerates billing, and creates a smoother patient experience at check-in.
Scheduling
Scheduling sets the tone for the entire revenue cycle. We align appointments with payer rules, provider requirements, and downstream billing readiness to prevent no-shows and authorization issues. Done right, scheduling reduces rework, improves patient preparedness, and protects revenue before care is delivered.
Insurance Eligibility
Eligibility errors lead directly to denials, delays, and patient dissatisfaction. We perform real-time eligibility and benefits verification, validating coverage, co-pays, deductibles, and financial responsibility upfront. By resolving discrepancies before the visit, we reduce downstream denials and enable faster, cleaner reimbursement.
See What Smarter RCM Really Delivers
With MedStat, every step of your revenue cycle is powered by intelligence, from eligibility to compliance. Our sixth-sense approach anticipates issues, prevents delays, and helps you capture more revenue with less friction. These are the results you can see, measure, and trust.
Who We Serve
Specialties We Serve But Not Limited To
Ambulatory

We support ambulatory care providers by streamlining revenue cycle operations to match the fast-paced, high-volume nature of outpatient services. Our tailored solutions reduce administrative burdens and enhance reimbursement rates, letting providers focus more on patient care and less on paperwork.
- Faster claims processing with reduced denials
- Transparent reporting and performance analytics
- Seamless EHR and billing system integration
- Improved cash flow and operational efficiency
Anesthesiology
Anesthesia billing is highly specialized, relying on precise time tracking, base units, modifiers, and the correct use of CRNA-related codes. We ensure compliance with payer rules while maximizing reimbursement accuracy for every case.
- Monitoring time units and base units for accurate billing
- Correctly applying modifiers and anesthesia type codes
- Navigating CRNA billing complexities
- Adhering to payer-specific conversion factors and guidelines
Emergency Medicine

We specialize in managing the complex and fast-paced billing needs of Emergency Departments. Our team ensures accurate coding, quick turnaround on claims, and compliance with ever-changing payer requirements to optimize reimbursement in this critical care environment.
- Real-time eligibility verification and pre-bill edits
- Expertise in high-acuity coding and documentation
- Reduced claim denials and faster payment cycles
- Scalable solutions for 24/7 operations
Endoscopy

We help endoscopy centers navigate the unique coding and billing challenges of procedure-based services. Our RCM strategies improve collections, minimize denials, and ensure proper documentation to maximize revenue without sacrificing compliance.
- Precision in procedural coding and charge capture
- Reduced billing errors and faster reimbursements
- Support for bundled payment models
- Analytics for procedure performance and revenue trends
Family Practice

For family practices, we offer comprehensive RCM support that balances the wide range of services with streamlined, efficient billing. From preventive care to chronic condition management, we help practices stay profitable and compliant.
- Support for diverse CPT/ICD coding
- Denial prevention and AR follow-up
- Simplified patient billing and collections
- Integrated scheduling and billing workflows
Gastroenterology

Our RCM services for gastroenterology practices ensure accurate coding and optimized reimbursement for both office visits and complex procedures. We help navigate payer policies and reduce revenue leakage across the care continuum.
- In-depth knowledge of GI-specific coding and modifiers
- Compliance with evolving coverage rules
- Better cash flow with clean claim submissions
- Detailed reporting for revenue optimization
RCM For Gastroenterology: Optimize Complex Procedure Reimbursements
General Practice

We provide general practices with efficient RCM solutions tailored to broad-spectrum care. Our support ensures steady cash flow, reduced administrative strain, and improved claim accuracy so practices can stay focused on patient wellness.
- Streamlined workflows for diverse visit types
- Accurate coding for preventive and acute care
- Reduced denials and quicker reimbursements
- Easy-to-understand patient billing solutions
Infectious Disease

Our RCM services for infectious disease specialists focus on the complexities of long-term care, diagnostics, and evolving treatment plans. We help ensure correct billing and optimal reimbursement in this highly specialized field.
- Accurate coding for complex patient conditions
- Effective management of prolonged treatments
- Real-time updates on payer policy changes
- Custom reports to track revenue trends
Internal Medicine

We help internal medicine providers manage high-volume, chronic, and preventive care billing. Our systems reduce claim errors and improve collections so practitioners can deliver consistent, long-term patient care without financial disruption.
- Expertise in chronic care and wellness coding
- AR management to prevent revenue leakage
- EHR integration for seamless billing
- Patient-friendly financial communications
Laboratory

We provide laboratories with fast, accurate billing processes tailored to high test volumes and frequent payer changes. Our solutions ensure labs receive timely payments while maintaining compliance and reducing rework.
- Automation to handle high test volumes
- Up-to-date coding for evolving test panels
- Denial reduction through payer-specific edits
- Detailed insights into reimbursement patterns
5 Must-Know Strategies To Boost Your Laboratory Revenue
How Streamlining Financial Data Management Boosts Lab Revenue
Neurology
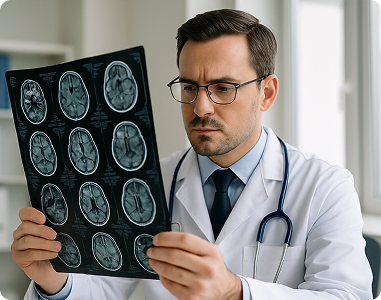
Neurology practices face intricate coding challenges that we simplify through expert RCM. From consultations to advanced diagnostics and procedures, we help optimize reimbursement while maintaining compliance with complex payer rules.
- Accurate neurological procedure coding
- Claims tracking for ongoing patient care
- In-depth reporting for practice analysis
- Prior authorization support for diagnostic services
Neurology Billing Mastery: Cut Denials With Precision Coding
OB/GYN

We support OB/GYN practices by handling both routine and complex billing needs, covering preventive exams, prenatal care, and surgical procedures. Our approach improves revenue consistency across all phases of patient care.
- Expertise in global maternity billing
- Surgical and procedural coding accuracy
- Timely reimbursements and denial management
- Patient education on billing and benefits
Orthopedics
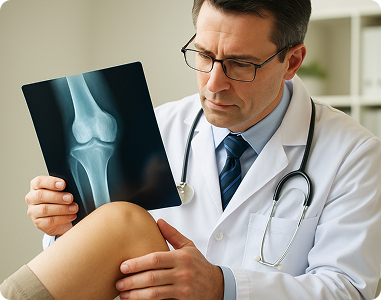
Orthopedic practices deal with complex procedures, modifier-heavy coding, and strict payer rules. We help reduce denials and improve reimbursements by ensuring each claim reflects the procedure’s full scope and specificity.
- Correct use of surgical and anatomical modifiers (e.g., 59, LT/RT, 22)
- Strengthening documentation to support intricate procedures
- Submitting claims aligned with payer-specific policies
- Avoiding audits with precise, compliant coding
Pain Management

We help pain management clinics with precise billing for interventional procedures, diagnostics, and chronic care. Our solutions reduce denials and improve reimbursement for services that require complex documentation.
- Coding expertise for injections and procedures
- Documentation review for compliance and accuracy
- Streamlined prior authorizations and appeals
- Improved cash flow with faster claim cycles
Podiatry
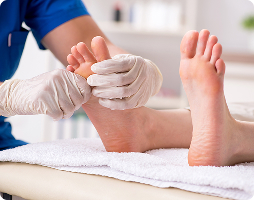
Podiatry practices benefit from our targeted RCM support for both medical and surgical services. We help ensure proper coding and timely payments across routine care and advanced foot and ankle procedures.
- Coding for wound care, diabetic foot exams, and surgery
- Patient eligibility and coverage verification
- Claims submission with minimal delays
- Compliance support for Medicare and private payers
Pulmonary Disease
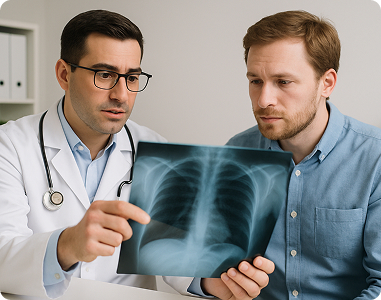
We assist pulmonary specialists in managing billing for complex, chronic conditions and diagnostic testing. Our RCM approach improves claim accuracy and keeps revenue flowing for practices dealing with high patient needs.
- Accurate billing for testing and treatments (e.g., PFTs, CPAP)
- Support for long-term care documentation
- Reduced delays with clean claim submission
- Real-time financial performance tracking
Radiology

Radiology billing requires clear separation of technical and professional components, plus meticulous documentation. We help radiology providers reduce denials and accelerate cash flow by ensuring coding and documentation are handled flawlessly.
- Managing global vs. split billing for technical/professional services
- Verifying and organizing referring physician orders
- Reducing undercoding and claim denials through detailed reports
- Streamlining claim submission for faster reimbursements
WHY LUMBAR SPINE MRI IS A HIGH-RISK, HIGH-OPPORTUNITY SERVICE LINE
Top Challenges In Radiology Billing and How RCM Solves Them
Surgery
We deliver specialized RCM services for surgical practices by managing pre-auths, global periods, and complex coding. From outpatient procedures to hospital-based operations, we support surgeons with optimized revenue capture.
- Precision in surgical and modifier coding
- Pre-op and post-op billing management
- Global period tracking and documentation
- Payer-specific rules and compliance support
Therapy

Therapy providers, from PT to speech and occupational therapy, rely on our RCM solutions for accurate service tracking and billing. We support high-volume practices with efficient workflows and fewer denials.
- Documentation audits to ensure compliance
- Real-time billing updates and claim status tracking
- Support for multiple payer rules and authorizations
- Transparent patient billing and collections
EMS - Ambulance

We help ambulance and transport services manage complex billing for emergency and non-emergency trips. Our team ensures proper documentation and compliance with federal and state payer guidelines.
- Accurate trip documentation and mileage billing
- Compliance with Medicare/Medicaid transport rules
- Faster payments through clean claim strategies
- Billing support for both ground and specialty transport
Urgent Care

We tailor our RCM solutions to the fast-paced environment of urgent care centers, supporting walk-in visits, point-of-care services, and rapid patient turnover with accurate and efficient billing practices.
- Coding for varied acute and minor procedures
- Same-day claim submission workflows
- Real-time eligibility and copay verification
- Integration with clinic management software
Top Challenges In Radiology Billing and How RCM Solves Them
Let’s Talk
Ready to See What Others Miss?
MedStat gives you the clarity, automation, and insight your practice needs to thrive.